-
Platform
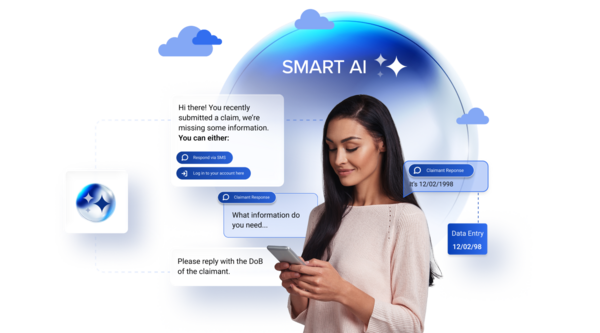
The Conversation CloudTM
The Smart Communications Conversation Cloud is the only cloud platform delivering personalized, omnichannel conversations across the entire customer experience.
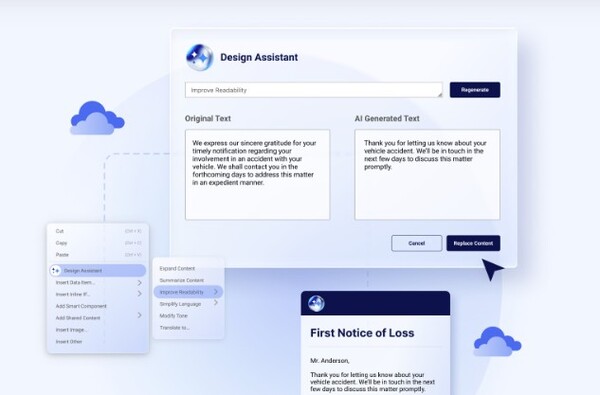
Explore the PlatformKey CapabilitiesCollect, Communicate, Collaborate and Coordinate — are bolstered by our strength in Integrations and Intelligence — enabling enterprises to engage in SMARTER customer conversations built for today and tomorrow.
Deliver SMARTER Conversations in the Cloud
Explore how enterprises can leverage a cloud-based, CCM platform to optimize the end-to-end customer experience.
Learn More -
Products
ProductsLearn more about our core products
-
Create and deliver personalized, compliant customer communications at scale.SmartCOMMConfront communications obstacles with pure-SaaS CCM Software
-
Turn static forms into guided, conversational digital experiences.SmartIQDesigned to tackle your most pressing forms-related issues.
-
Archive and retrieve communications securely with cloud-native speed.
-
Orchestrate real-time, compliant interactions across every channel.
-
Simplify and standardize trade and relationship documentation workflows.
-
-
Industries
IndustriesMaking customer conversations SMARTER when it matters most
-
Financial ServicesEngage in faster, frictionless financial Interactions.
-
InsuranceEnable secure, scalable, business-driven policyholder engagement.
-
Healthcare PayerTransform the healthcare experience with digital and interactive conversations.
-
Healthcare ProviderAccelerate omnichannel patient engagement with guided digital journeys.
-
-
Partners
PartnersIntegrate seamlessly with the best in the industry

Deliver SMARTER Conversations via Our SmartPARTNER Network
We work with best-in-class technology and consulting companies to offer integrated solutions that complement our family of products.
-
Resources
ResourcesExpert advice and tips to make your conversations SMARTER
2026 Trends Research
Insights from 20+ partners and analysts on optimizing customer engagement in 2026.
-
About Us
About UsLearn more about our company, our leadership and how were growing the team!
- Request a Demo